Emergency medicine doctors welcome public protests over hospital overcrowding
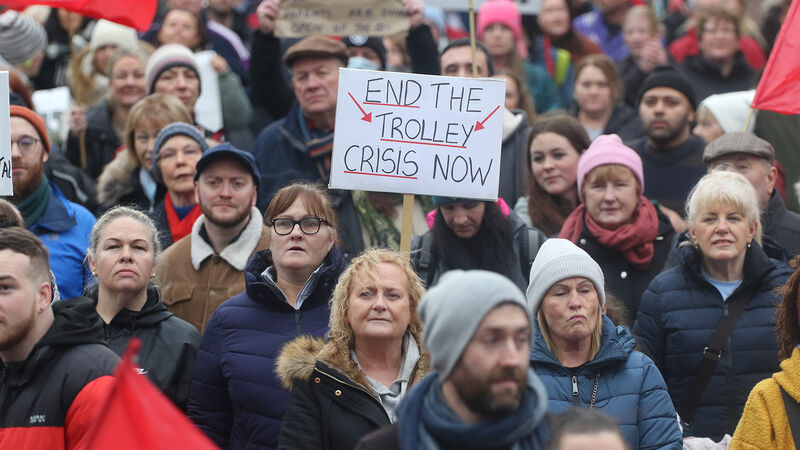
Consultant in emergency medicine Fergal Hickey said: 'We welcome the fact that the public is no longer prepared to tolerate the unacceptable situation which has been foisted on both patients and staff in emergency departments.' Picture: Brendan Gleeson
Protests against hospital overcrowding have been welcomed by the Irish Association of Emergency Medicine, which called for proper funding around hospital beds to address the crisis.
Among the national protests, an estimated 11,000 people marched in Limerick to highlight concerns.
Lunchtime News
Newsletter
Get a lunch briefing straight to your inbox at noon daily. Also be the first to know with our occasional Breaking News emails.












