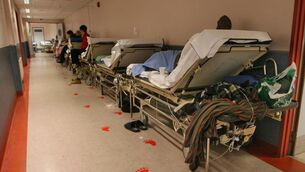
Medics work 120k hours overtime in 5 months

New HSE figures show 304 medics at Cork University Hospital worked the significant overtime to fill chronic service gaps between July and November, with doctors warning the strain is putting patients at risk.
According to details obtained by trade publication the Medical Independent, over the five-month period, 304 junior doctors at CUH worked a combined 124,779 hours of overtime.
Lunchtime News
Newsletter
Get a lunch briefing straight to your inbox at noon daily. Also be the first to know with our occasional Breaking News emails.