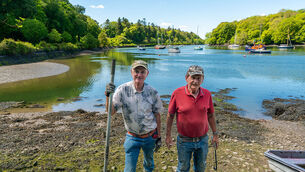Assisted dying: Knowing when it is time to go

Less than a month into their relationship, Vicky Janssens (right) discovered lumps in her neck and doctors later confirmed that her cancer was back. Garret Ahern (left) said: "I wasn't going to walk away from this woman who I loved."
Time flew so much on their wonderful first date that he nearly missed his train home. But it was as if time stood still on their final day together as he watched the life ebb from the pain-wracked body of his terminally ill wife after she availed of an assisted dying procedure in Belgium.
Driven by the memories of those two days which bookended their loving relationship, grieving husband and father Garret Ahern is now campaigning to legalise assisted dying here — a law which would have meant that his beloved wife, Vicky Janssens, could have died at home in Cork the way she wanted.
As the joint Oireachtas committee set up to examine this emotive issue prepares to resume its public hearings next week, Garret has decided, even if it means he could face prosecution, to speak publicly for the first time about his wife’s agonising cancer journey, about her decision to avail of an assisted dying procedure in her native Belgium, of how he travelled with her on her final journey and how he felt isolated and alone as he held her hand as she died in a friend’s house, and about how he hopes the time is right now for Ireland to have a mature and rational debate about how we approach death and dying.
Belgian-born Cork-based UCC lecturer Vicky Janssens, a double mastectomy cancer survivor, was about to be discharged from her oncology aftercare service when she met Limerick man Garret Ahern online in 2018.
Both divorcees and both parents, they enjoyed their online rapport and Vicky, a lecturer in Greek and Latin, invited Garret to Cork for their first date one beautiful summer’s day in June.
“I forgot to bring any sunscreen with me, and it was one of the hottest days of the year. So I ended up with really bad sunburn,” Garret recalls. “That’s certainly one of my memories of that day. But not the fondest memory of that day. The connection between Vicky and I was instantaneous.”
He smiles as he recalls how they ate in Electric, overlooking the southern channel of the River Lee in the heart of the city, and of how they strolled around the grounds of UCC’s sun-dappled campus, the smell of freshly cut grass hanging heavy in the air.
“I didn’t go to university myself so being on the grounds of UCC — it was a first for me and it was magical,” he says. “We chatted, the hours slipped away — I very nearly missed the last train back to Limerick — as did every hour that we spent together for the rest of the time we had together.”
A week later, Vicky invited Garret to Cork again to attend her birthday party at her home, where he met her friends, neighbours and colleagues.
“I found my tribe,” he says. “We had similar views, we could talk about a similar range of subjects, we had similar outlooks on the world. And from there began an inevitable romance that led to an enduring love and ultimately to marriage.”
But that would come later. Garret knew from very early in their relationship that Vicky had had a double mastectomy, and had gone through five years of oncology follow-up cancer-free.
He also knew from early on that Vicky wasn’t interested in marriage — she’d made that quite clear. She said she liked him a lot, and that she would put up with him, but she would never marry him. “I knew exactly where I stood,” Garret says, with a grin.

Then a week after her birthday, the whirlwind romance came crashing down when Vicky discovered lumps in her neck which gave rise to concern. Doctors later confirmed that the cancer was back, and had metastasized to her lymph nodes.
“It became apparent that she was going to die a lot sooner than she thought,” Garret says. “So we are less than a month into our relationship and she says ‘I will completely understand if this is not for you’.
“We could be starting on a road here and it may not end well.” But he says: “I have never backed down from doing the right thing in my life. I feel that had I walked away in an act of self-preservation, that it would lessen me as a man, lessen my character.
“I'm a union rep, a Red Cross volunteer, I worked in a suicide prevention charity in Limerick as well. I always stick up for the underdog. So I wasn't going to walk away from this woman who I loved, and who now had a need. And I had the strength of character to support her and her daughter.”
As her pain increased and the illness became terminal, Vicky changed her mind about marriage and popped the question. Without hesitation, Garret said yes and the couple married on June 12, 2021.
“You have to overcome the fear,” he says. “You could live every day in anxiety with this if you wanted to, every day paralysed with fear. Or you could say ‘to hell with it’. Let's get out there and do it.”
And they did. They put thoughts of death and dying to one side and got on with living. “The thing about living with a terminal illness is that you live your life every day because you realise those days are finite,” Garret says.
“So we did endeavour do our best — we travelled, we got out into nature a lot. Vicky would collect seashells on the beach. These things filled her with joy and happiness.” But the cancer spread.
“We were lucky for a good number of years. But then it catches up,” Garret says. “Vicky started to realize that the clock was ticking a lot louder and then we began to have the conversations about her end of life and her wishes around that.”
Cancer had haunted Vicky Janssens since her teenage years. In an interview published in this newspaper in 2014, a year after her double mastectomy, she said the idea of getting cancer had been in her mind since she was 17, when her mother was diagnosed with the disease.
“In a way, it was sort of a relief when I got my diagnosis, it was like I was expecting it,” Vicky explained. Her great-grandmother and grandmother had both died of breast cancer. Her family history left her with a high chance of a genetic predisposition towards cancer.
She was diagnosed with breast cancer in 2013 and faced it bravely. Now, just as she found love, she was facing another cancer battle. Following the removal of her lymph nodes and radiotherapy treatment, Garret says it became clear from the three-monthly scans that they were on “a trajectory that will lead to her death”.
A shadow on her lung which they initially thought could be scarring from the radiotherapy following the double mastectomy was later confirmed as cancer that had metastasized to her lungs. She was on oral chemotherapy and taking a cocktail of highly expensive drugs which kept the condition at bay.
“But Vicky knows that it won't keep the condition at bay forever. And the prognosis for somebody with Vicky’s type of cancer was two years,” Garret says. “Our lives revolve around going for these scans and waiting for results.”
The medications had side-effects which limited Vicky’s ability to live a full life and then came the bombshell — the cancer had now spread to her liver. She was told the disease path progression was liver, stomach, bones and then brain.
By September 2022, Vicky was having trouble eating and swallowing and within weeks, she was vomiting during almost every meal. “The joy is being sapped away from our lives by this. She's weak. She's tired. She's sick. She's worried. She knows there is something going on,” Garret says.
She had another scan last December and told her husband that if the news was bad, she didn’t want any more chemotherapy, but Garret suggested they wait for the results and decide then. And they were able to tell from the face of the medic delivering the news that their worst fears had been confirmed.
“We had been in this rodeo many times. We knew when they were struggling to present something." The doctor told them the disease had changed and had progressed to the lining around Vicky’s stomach and that the tumours in her liver had increased.

Vicky refused chemotherapy but Garret convinced her to talk to her consultant, who persuaded her, against her wishes, to give treatment one more try. She underwent three or four sessions of intravenous chemotherapy in January but found it was just too much, and the pain worsened.
“So now she's in excruciating pain,” Garret says. “She's losing weight, she can’t eat, she’s losing her hair. She's angry — angry that her life is being taken away. She’s angry at cancer, she's angry at dying.
“She would be in for chemo every week. Then sick for two or three days afterwards, and then she’d start to come around, and would then start to get anxious about having to go back in again. And she just said ‘no’ — she wasn't going to do it, she couldn’t do it anymore.”
They told the oncology team that they were stopping treatment, and Vicky became the patient of a palliative care service. But Garret says some of those pain medications just didn’t work. She described the pain as like have a rat gnawing at her insides, all the time.
“We had a fantastic relationship — an abundance of love. But I can't hold my wife, I can't lie next to her in bed because it's causing her too much physical pain. And it's causing her too much psychological distress,” he says.
He slept on a couch downstairs for weeks — a period he describes as hugely traumatising and distressing. “I'm the father of four daughters, and I would do anything for them but I can’t do anything for my wife,” he says.
“I'm not sleeping. Several times a night, I come upstairs to check on Vicky. She’s almost always awake and I say ‘can I get you anything? Sometimes it's ‘can I have a bowl to get sick in’, sometimes it’s ‘can I have some water’, but most of the time it’s ‘no, leave me alone’.
“And I sit by her side, I hold her hand, stroke her hair and after a very short few minutes she says just go, just go. So I go back downstairs and feel hopeless and lost.”
Early in her cancer journey, Vicky filled out ‘think ahead’ forms, setting out her wishes on everything from the flowers and songs at her funeral service, to the limits to any resuscitation efforts in the event of a life-threatening medical emergency.
But as the cancer progressed, her thoughts soon turned to managing the manner and timing of her own death. “Vicky had clearly said that if she was in trouble, if she was unconscious, if she was dying, she didn’t want people to ventilate her, she didn't want people to use a defibrillator,” Garret says.
“This is not an easy conversation to have with your wife. It is the responsibility of medics to do everything they can to immediately save a life. But she's telling me and stating in this form, which is signed and witnessed, that she doesn't want that and that I’m to battle on her behalf to ensure that that doesn’t happen.
“Her reasonings behind it were sound. It wasn't that she just wanted out or wanted to die in the event of something catastrophic happening to her. She didn't want to linger on in pain and in suffering.
The issue was discussed, but then parked for a year or two while the couple got on with living, and Vicky continued her treatment. But by September 2022, when she was finding it increasingly difficult to eat or swallow, the discussions about managing her death began again.
“It is not because you've had a bad day at the office that you decide to take on something like this. She probably felt that she was already too much of a burden and didn't want to load it on,” he says.
Vicky had asked the palliative care team if medicinal cannabis might work but they said it wasn’t indicated for her condition. And one day, after one of the nurses left the house, Vicky turned to Garret and said: "What if I just drank all the morphine that I have in the house?"
A volunteer with The Samarians some time ago, and a volunteer with a suicide prevention group in Limerick which patrolled the river Shannon, Garret often met people in distress.
For some, a chat was enough, for others, a friendly word, an understanding ear, or an arm around the shoulder was enough but he knows they couldn’t get to everyone.
“I said to Vicky that suicide rarely works out the way people plan, and most people who survive said they regretted it — so don't do it,” he says. But in mid-February, she tried it anyway.
That evening, Vicky goes to bed at 8pm. Garret checks her at 9pm. The lights are on in the bedroom and he can see the pain etched across her thin greying face.
“I have watched my wife’s decline over a number of years but over the course of the last few weeks, she was really deteriorating. She was turning into a shell and you can see the pallor of her face, and the pain in her face,” he says.
She tells him she is ok, and then says something he hasn’t heard for weeks. “She tells me that she loves me and her daughter very much. That's something that I used to hear all the time but hadn't heard for weeks. So I was happy. I thought maybe she's finding some peace with her condition,” he says.
He goes downstairs to watch some TV, and before he turns in for the evening on the couch, he checks her again at around 11pm. “She is sleeping soundly. I can hear her those deep relaxed breaths and I think thank goodness she’s found a restful night's sleep,” he says.
He goes back downstairs and falls asleep on the couch, waking at around 6am. “And so begins the maelstrom,” he says. “I go upstairs and there's a different scene. Her breathing is rasping and irregular.
“I turn on the lights and she's in bed. Her lips have a bluish pallor, she is cyanosed and there are two empty bottles of morphine and tablets by the side of the bed.
“So I take her pulse rate, I count her level of respirations, I count her breaths per minute. I make the guess that she has taken these (medications) at 9pm after I went downstairs.
“It's now 6am and I'm trying to scramble all the knowledge that I can think of, whether or not the fatal effects of these opiates has passed.” He administers a few rescue breaths before calling the emergency services.
Paramedics arrive within five minutes and Vicky is rushed by ambulance to Cork University Hospital, with Garret accompanying her, where doctors begin treatment.
There's a man in the cubicle next to them who has suffered a serious head injury and is in clear distress. He's screaming and has to be held down by security guards.
Garret is questioned about Vicky’s global cancer and her treatments and it’s touch and go for her that day. But within 24 hours, she begins to come around. She opens her eyes, and holds Garret’s hand, and is later moved to an examination room in the ED.
“It's a commonplace story — it's chaotic, it's overcrowded, it's people on trolleys in corridors,” Garret says.
She’s eventually moved to a ward where a healthcare assistant sits nearby keeping her under observation. There are other patients in the ward with complex needs. The results of medical tests come back and show that Vicky’s organs haven’t been damaged, but that the cancer is advanced.
A psychiatric assessment follows, and Garret says it concludes that Vicky had a desire to end her suffering, rather than a desire to end her life. She pleads with him to take her home. She is discharged a few days later.
Garret says: “She said she just wanted to go home and sit in her garden and have a cup of tea. But she can’t sit without being in pain. No amount of cushions or positioning can make her comfortable. And the sips of water, sometimes stay down, sometimes don't.
“She wanted to avoid the worst of the healthcare system. And she got the absolute worst of the healthcare system.”

And then comes the toughest question Garret says he’s ever been asked. He reckons she’s spent weeks preparing. “She tells me that she has a difficult question for me and that there's no right or wrong answer. Or that I don't have to do this if I don't want to,” he says.
“She says she has decided that she is going to Belgium. She has booked the Airbnb. She has booked the flights. She’s booked a consultation with a doctor. She has already had some Zoom consultations with a doctor and that she's going with or without me.
“And this is not an ultimatum. This is just a statement of what’s going to happen and that if I can’t do this, that’s ok but she's doing it anyway. It's organised and the train is set in motion. She just needs to ring a friend tonight to let her know if she’s coming over or if I’m going with her.”
Reliving that experience now is traumatising still, he admits. “It was like being in a car crash. Everything stops and slows down,” he says. Nothing is real, except Vicky telling me this, presenting this to me.
“And how could I here, at the final furlong, how can I abandon her now? How can I let her die without me being there to hold her hand. So of course I agree to go.”
It’s a bright spring April morning when Garret and Vicky take a taxi from their home to Cork Airport to board a flight to Schipol in Amsterdam. Vicky waves goodbye to her daughter at the house knowing she will never see her, or home, again.
“I’m crushed, I’m a shell of who I was,” Garret says. I'm just going on autopilot at this stage. Because even if I had said ‘I can't do this’, she would have got into the taxi by herself. She was so determined to end this.”
A few days before, a medical drain has been removed from her abdomen, but the wound still oozes. Garret recalls being worried that the aircraft cabin pressure on the flight might cause it to ooze more so he has applied an extra-large dressing, “a battlefield wound dressing”, to protect against that.
The couple is met at Schipol by some of Vicky’s friends, who drive them to Antwerp in Belgium, where the right-to-die law was adopted in May 2002.
Read More
“They cry and they hug, they speak to each other in Flemish, they greet me in English,” Garret says. "They've pretty good English but they’re speaking in Flemish in the car.”
Later in the journey, Vicky says she’s too tired to translate for Garret anymore and he feels like an outsider. “They make efforts to talk to me, but 95% of conversations are in Flemish, as it was for the entire 10 days,” he says.
They arrive at their Airbnb apartment and settle in. Garret tries to make Vicky as comfortable as possible. She asks for yoghurt, custard and water and when he comes back from the shop, and she finishes eating what she can, he helps get her ready for bed.
“I take off that wound dressing and you could wring it out like a sponge,” he says. Once Vicky is settled, he goes upstairs to the living room, sits on a little balcony, and looks across the busy city in the fading spring light.
He says:
The next day, they attend a consultation with ‘the presiding GP’ — one of the many medical practitioners in Belgium who help people die at home under their right-to-die laws.
Under Belgian law, patients qualify for euthanasia only if they have an incurable illness and experience constant, intolerable physical or mental suffering that cannot be alleviated.
They also have to expressly repeat an explicit request for assisted death, which must be proven, thoroughly thought-through and not subject to any outside pressure.
Vicky has already forwarded her medical files and the GP concurs that she is terminally ill, that she is in incredible pain, and that she is a candidate for euthanasia. The law requires a second opinion, with a consultation scheduled for the following day.
The couple returns to their accommodation that night and wait. “It’s not like you can make plans to go out for dinner. There's nothing to speak about anymore. Because it's just death, death is in the room with us,” Garret says.
“And we’re both dealing with it, and with our relationship, with what's coming. We're so numb and in shock that we can't really interact all that much.”
Vicky’s parents call that evening to say their emotional goodbyes. The next day, Vicky and Garret attend a consultation with the second GP, which is conducted again in Flemish. The GP asks Garret if he understands what's going on. He says he does.
The GP then places an order for the required medications for the assisted dying procedure with the pharmacy nearest to where it is scheduled to take place in just two days’ time.

The couple returns to their accommodation and wait again. “We try to say all the things that needed to be said. Even though I had said it a thousand times, there’s always room for one more I love you,” Garret says.
On Friday, April 21, the couple leave their apartment at 10am and arrive soon afterwards at the house of a friend of Vicky’s where she will die. Four of her close friends are there. There are flowers in the house. It is a beautiful sunny day and Vicky sits in the garden for a while.
There are some precious moments as they wait. A beautiful white cat walks across the grass. Vicky spots a bee landing on a flower. She always liked bumblebees and she turns to Garret and smiles. He smiles back. They do not speak. There is no need.
Vicky is very tired now and doesn’t speak in English much anymore, and Garret feels alone. “I am the supporting actor. I don’t speak the language. I am completely removed from what is happening,” he says.
He recalls a sense of dread and numbness in those final hours before the procedure, but also an overpowering sense of grim resolve to see this through. “Over the five years that Vicky and I were together I have never let her down and I’m not going to let her down now,” he says.
“We just need to keep going for another few hours but I am not part of the scene. I have been removed from the scene by culture, by not speaking the language. I felt excluded, on the outside.”
A palliative care nurse arrives at the house at 1pm and has another consultation with Vicky — again in Flemish.
Garret says:
Vicky is now sitting on a couch in a downstairs room and an IV drip is inserted into one of her arms. She feels better within minutes. “She knew her pain was coming to an end and all she wanted was for the pain to come to an end,” Garret says.
Doctors arrive at 2pm and some of Vicky’s friends become upset and leave the house for a while. Swabs, medical drapes and medications are laid out on the kitchen table and a second consultation with the presiding doctor takes place.
He explains what is about to happen — that he will administer a general anaesthetic first through the IV, followed some minutes later by a muscle relaxant.
He tells Garret that Vicky has made it clear to him that she wants this procedure to take place. He tells Garret that if he tries to stop the procedure, or says ‘no, don’t do this’, that he has to follow Vicky’s wishes. He asks Garret if he understands the position.
The GP then asks him if he wants to say anything to Vicky now to try and change her mind. “That would have been pointless,” Garret says.
The GP then administers the anaesthetic.
Vicky says: “Wow, this is great. I could really get used to this.” She smiles, and then she laughs. And Garret laughs a little too, before his wife loses consciousness.
The GP gives them a few moments together, alone, before Vicky’s friends come into the room, kiss her goodbye, and leave again. The presiding doctor is joined in the room by another doctor and the palliative care nurse and they tell Garret that they are proceeding now to inject the muscle relaxant.
He says:
“At that moment I felt relief because once the general anaesthetic had been administered the furrows and signs of pain that were etched on her face and had been for many months were gone. At least it was pain-free peace in the moment before she died.
“And after her death there was relief that she had gotten what she wanted and that her pain was gone, that she wouldn’t have to endure anymore. I wanted for her wish to die to happen because the pain was so much.
“I would’ve given her a kidney. I would’ve chopped off my right arm if I thought it would have kept her alive but nothing anyone could do could take away that pain.
“All she could do was wrestle back control that she could end her life and her pain at a time and in a manner of her choosing, with as much dignity as possible. And she did. So I was proud of her and relieved that the pain had ended.
“And then comes the devastating reality of life without her, having to pick up the phone to my stepdaughter and tell her that it has happened, that her mum is dead. This is so traumatic I don’t know how I’m ever going to recover from this.”
Vicky's daughter flew to Antwerp a few days later to join her stepdad at a funeral service, which was conducted in Flemish. Heartbroken and exhausted, Garret felt lost and adrift, understanding little of what was being said.
He had initially indicated to the undertakers that he didn’t feel he would be able to speak at the service, but a few hours beforehand, he found the strength and told them that he would now like to address the congregation briefly, to pay tribute to his wife.
But he was told that the service running order had already been finalised, and that his wishes could not be accommodated at “this late stage”. He never got the chance to deliver a eulogy.
Vicky’s remains were cremated a few days later after Garret and her daughter flew home to begin rebuilding their shattered lives.

Two weeks passed. Then one morning, an email from the undertakers landed in Garret’s inbox, with an invoice attached, informing him that his wife’s ashes were ready for repatriation, and requesting payment.
One of her friends had already agreed to transport the ashes back to Ireland. That friend carried Vicky’s remains in her hand luggage on the aircraft, placing them carefully in the overhead compartment for the flight to Cork.
Garret says he hasn't had the strength since to scatter them as she wished — on a favourite bench overlooking the sea near the Parknasilla Hotel in Kenmare, Co. Kerry.
“She wanted them to be scattered in spring or summer, but I just wasn't ready this year,” he says. “I hope to do it next year. And in the fullness of time, my ashes will be scattered next to hers.”
Garret has decided to speak publicly about Vicky’s death in the hope of changing the law on assisted dying in Ireland.
“Our story is tragic. It's heartbreaking. And the stress and the trauma that you have to endure traveling to Belgium, having the procedure carried out in Belgium and having to stay in Belgium for the funeral afterwards is not something that I would wish anyone to have to go through,” he says.
“I’m not doing this to seek publicity or the limelight. But if the legislation in this country can be changed to facilitate, under very strict conditions, the dignified ending of a person’s life, and the ending of their pain and suffering, I think it will have been worth it.
He is conscious that people may view the introduction of assisted dying in certain conditions as a slippery slope, and risks opening the door to a liberal form of euthanasia. But he believes the right legal, medical and ethical safeguards could be put in place to protect against an abuse of the system.
“I am not in any way advocating that the elderly, people with disabilities, or people who do not wish to die in this manner, that they should be in any way coerced into this,” he says.
“If a person, no matter how serious their illness, can find joy in their life, for however long that life is going to last, for however long their health condition allows that life to last, they should certainly be allowed to live that life to its natural conclusion, with all of the excellent healthcare supports that we have in place in this country.
“This is about choice.” He still suffers from flashbacks from the overdose, and from some of the cruel things Vicky said to him when she was in excruciating pain, and he says he feels guilty for not trying hard enough to talk her out of it.
“But I couldn't talk her out of it. I couldn't find a counter-argument to the very rational well-considered decision that she had made,” he says. “I tried. I tried. But my argument was a strawman. I knew we didn't have the strength of Vicky's conviction.”

He knows this will be a multi-faceted debate, with various medical, ethical and religious views to be considered from a wide range of interest groups, but he feels the time is right for Irish society to have the conversation, and that if the matter is too big for legislators, then perhaps the question of introducing assisted dying in Ireland should be put to the people.
“I don’t want the limelight. I would give anything to have this burden lifted from me,” he says. “But it’s mine to carry. I can go to my deathbed, whenever that may be and in whatever manner that might be knowing that I've done my best for a cause that I believe in.
“I’ll do whatever it takes for as long as it takes, or for as long as my strength holds out, because this seeming facade of competence is paper thin — there's a broken man behind this.
“Not a day goes by without overwhelming grief. Not a night passes without nightmares. So I just have to keep going to the end, or until I collapse. Let's hope I have the strength to see this through.”
Available support:
- Pieta House 24-hour freephone crisis helpline 1800 247 247 or text HELP to 51444
- Samaritans 116 123