Over 75,000 people leave A&E without ever being treated
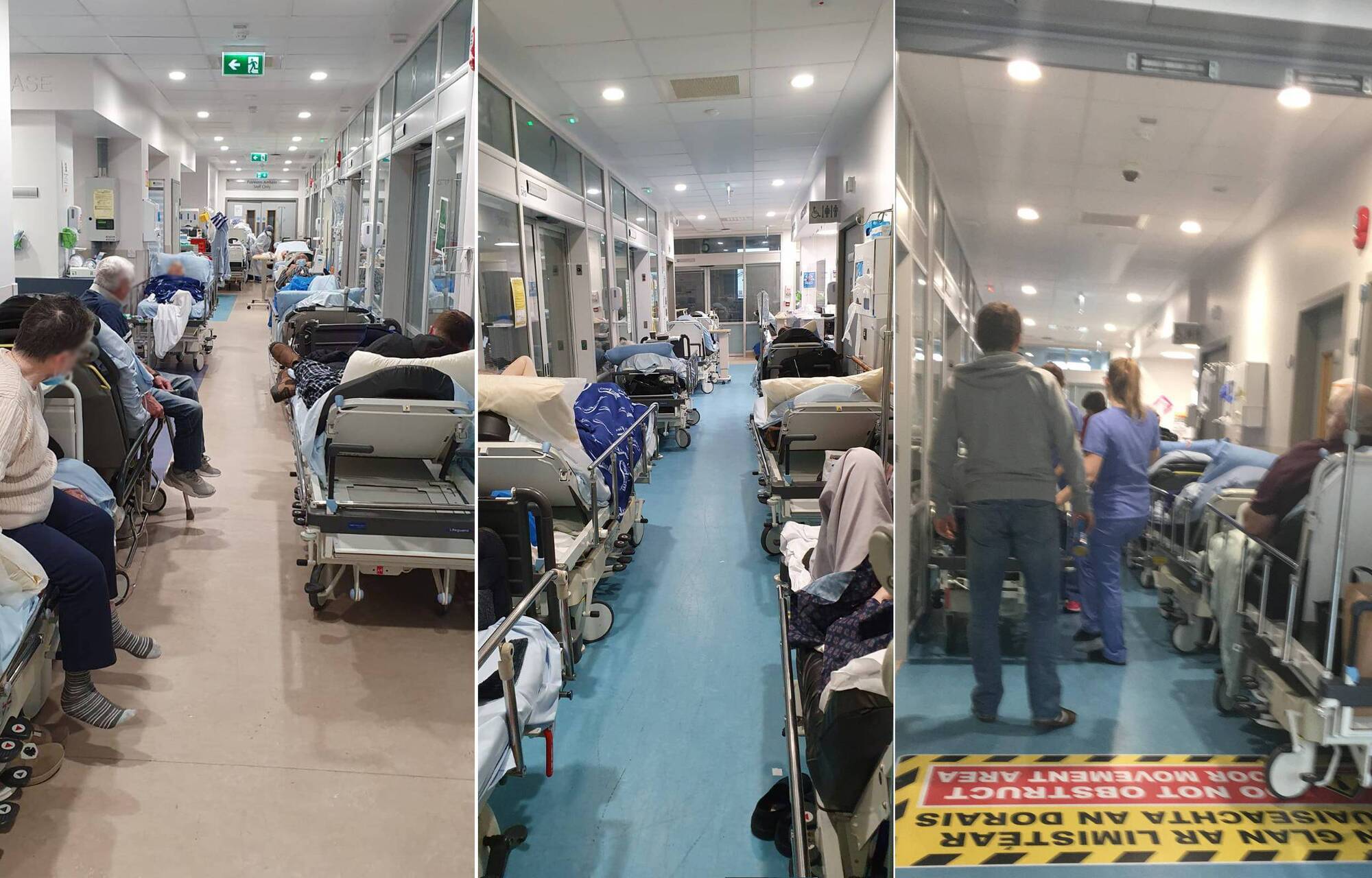
More than 75,000 patients walked out of A&E departments last year without ever being formally discharged or finishing their treatment.
More than 75,000 patients walked out of A&E departments last year without ever being formally discharged or finishing their treatment.
That included at least 3,400 cases involving sick or injured children presenting for treatment, although those figures are even higher due to data being unavailable for some months because of a cyberattack on the HSE.
Lunchtime News
Newsletter
Get a lunch briefing straight to your inbox at noon daily. Also be the first to know with our occasional Breaking News emails.