Tackling Covid-19: What we can learn from the 1918 Spanish flu?
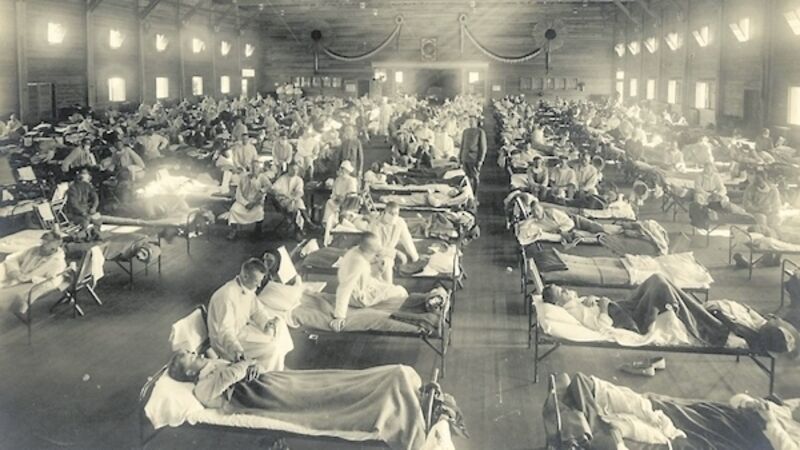
People consistently make a comparison: the 1918-1919 influenza pandemic, the ‘Big One’, against which other epidemics of respiratory illness are measured.
It killed upwards of 50 million people, according to the World Health Organisation — although we will never have a definitive number as death registration was then patchy in many parts of the world.










