Watch: Let’s not sugar coat our diabetes epidemic
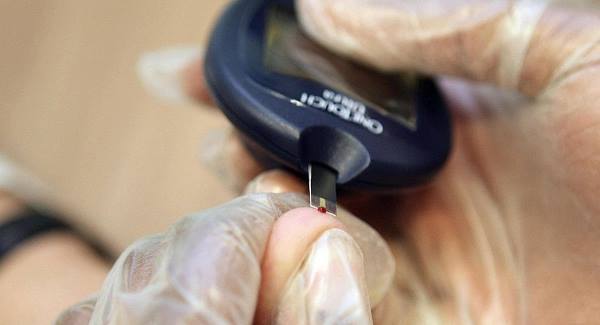
The International Diabetes Federation (2013) estimates that there are 207,490 adults with diabetes in Ireland (6.5% prevalence).
The good news is that we are getting better at treating patients with diabetes.







