Emergency department overcrowding 'breaches human rights'
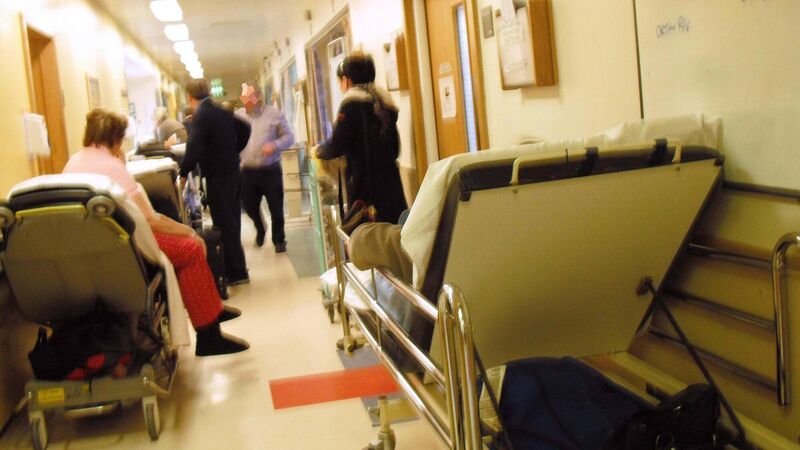
Patients on trolleys at Cork University Hospital. Overcrowding in acute public hospitals is putting patients at risk of harm and 'breaches their human rights', according to the Health Information and Quality Authority.
Emergency department overcrowding in acute public hospitals is putting patients at risk of harm and “breaches their human rights”, an unpublished paper by the State’s health and safety watchdog has warned.
A record 118,367 patients waited for a bed on trolleys in 2019, according to figures by the Irish Nurses and Midwives Organisation, which is generally accepted as the measure of emergency department overcrowding.










