Skin Nerd: Truth vs myth for World Psoriasis Day
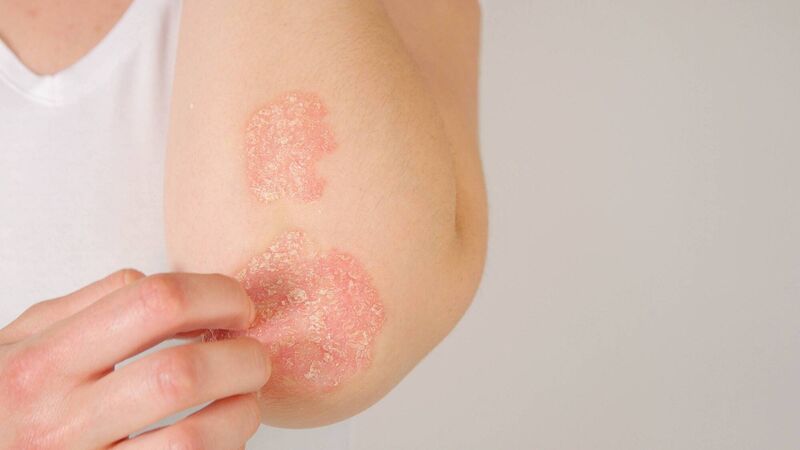
Skin Nerd: Psoriasis is treatable - and the Skin Nerd has advice and mythbusting aplenty
Life with a skin condition can be tough enough but things become even more complicated when battling through hordes of misinformation.
The most important thing to do if you suspect you’re suffering from psoriasis, or any skin condition, is to book an appointment with your doctor to discuss your symptoms and to get accurate advice on how to care for your skin.
As an additional guide, this week I separate fact from fiction when it comes to psoriasis.
Like most skin conditions, Psoriasis manifests in a number of ways and to minimise the skin disorder to just dry skin is a grand understatement.
Whilst psoriasis can be itchy and cause the skin to shed flakes (like dry skin), there’s a big difference between occasional dryness and Psoriasis, which is a medically chronic, inflammatory skin condition. Those with psoriasis have increased production of skin cells. Usually, skin proliferation, which is when skin cells reproduce and mature, takes around 28 days.
However, in those with psoriasis, skin cell proliferation is much faster and only takes around 3 to 7 days. This causes a build-up of dead skin cells on the surface of the skin, which results in red, raised (and often itchy) patches of skin – often referred to as “plaque.”
The difference also lies in the treatment of psoriasis versus dry skin. Whilst a hydrating lotion may be able to manage the surface-level discomfort of dry skin, treating an autoimmune skin disorder such as psoriasis can be trickier and require the use of medication and professional treatments.
Both psoriasis and eczema can result in itchy, red skin but there are many differences, including their underlying causes. Psoriasis is an autoimmune disorder, meaning that your immune system (whose job is to protect us from disease) accidentally attacks healthy skin cells and causes damage to the skin.
In the case of psoriasis, this results in the skin cells multiplying too fast. Eczema on the other hand, is usually caused by genetics and environmental factors. The symptoms can be different, too: Psoriasis causes thicker, red patches of skin (plaques), whereas eczema causes more of a standard itchy rash.
The most common form of psoriasis is plaque psoriasis, which affects 80% to 90% of the people who have psoriasis. Plaque psoriasis is characterised by thick red patches of skin that have a white or sliver scaly layer. The patches appear anywhere on the body and can vary in size.
There are four other common types of psoriasis:
- Guttate: Symmetrical eruptions that are drop like with a small presence of scales usually on the trunk or limbs.
- Flexural (also known as inverse): Presents as smooth looking plaques and can affect under the arms, under the breast or groin. This may be more predominant in the elderly.
- Pustular: A rare but potentially more serious form. Yellow pustules develop with an erythamous (inflammation) background.
- Erythrodermic: Inflammatory dermatitis that involves almost all of the skin's surface (sometimes more than 90%) Each type has unique treatment and subsequently requires individual treatment and care.
Psoriasis presents as red, dry and flaky patches of skin which can appear anywhere on your body – although elbows, knees and lower back are common hotspots, along with the scalp.
However, psoriasis can also affect beneath the surface of the skin, with some hoomans developing psoriatic arthritis, which also causes skin plaques, joint stiffness and swelling.
Alongside the physical symptoms, psoriasis can also affect your mental health, with many reporting depression and anxiety alongside their skin condition.
A harmful myth is that psoriasis is caused by poor hygiene. This is perpetuated by the fact that some people living with the skin condition often report feeling and looking ‘dirty’ when their plaques leave behind skin flakes.
I urge you to avoid this negative trail of thought as much as possible. Psoriasis is not caused by how often you shower or which soap you use to cleanse your body, in fact, over washing can actually make the flaking worse!
Instead follow a gentle, skincare routine using products designed for your skin type or as recommended by your skin specialist.
Another common misconception is that psoriasis is spread through close contact – in fact, 27.3% of hoomans in a recent study thought that the condition was contagious.** This isolating stigma is pure fiction and should not deter you from entering the swimming pool or hugging your friends at ease. Psoriasis is a non-infectious inflammatory dermatosis and doesn’t spread through touch.
Something that can cause psoriasis is genetics. Although it’s still unclear how large of a role genetics plays in the development of psoriasis, it has been found that you’re more likely to suffer from the skin condition if one of your parents has it – even more so if both of your parents do. In fact, you have a 41% chance of developing psoriasis if both of your parents have it.
Treatments cannot cure psoriasis permanently – however, there are treatments and ways of managing the condition that can bring relief, reduce inflammation and lessen the appearance of dry patches.
Adopting a consistent skincare regime is important. Take a gentle approach with your skin – which includes avoiding scrubbing and bathing in warm (not hot) water. I also recommend tapping your skin dry with a towel instead of rubbing and moisturising regularly to lock in hydration and keep any itchiness at bay.
If you get psoriasis within the scalp, this can be extremely itchy but can be eased using a medicated shampoo containing zinc or salicylic acid to help break down dead skin cells that are accumulating on the scalp.
Where topical treatments are concerned, your doctor might prescribe a cream, antihistamine or ointment that contains vitamin D analogues. These work by slowing down rapid skin cells production, which reduces the amount of dead skin cells building up and patches forming on the skin. Corticosteroids may also be applied directly to the skin to bring down inflammation and irritation.
The steroids come in different strengths with the strongest formulation only available as a prescription from your doctor. If topical treatments don’t seem to work, a treatment called phototherapy can be used. The process involves exposing your skin to types of ultraviolet light.
Coal tar therapy, which is rich in anti-inflammatory and anti-scaling properties, has been used for more than a century in dermatology and is mostly used for short-term scalp psoriasis too. Along with medications and topical care, lifestyle adjustments such as eating a healthy diet, avoiding smoking, and managing triggers such as emotional stress can help with psoriasis.
Skin icing is a cryotherapy treatment in which the skin is exposed to extremely cold temperatures for a limited amount of time (usually several minutes). It is said to have a variety of skincare benefits, including brightening the complexion, tightening the skin, and soothing redness.
The concept of using ice to reduce undereye puffiness isn’t new but the sudden influx of ice-based beauty tools is encouraging us to take matters like swelling, fatigue and dullness into our own hands. Granted the maraca-style cryoglobes can look gimmicky but there is a science behind this age-old trick.
What is happening here is vasoconstriction - applying cold to the surface of the skin tightens up those blood vessels thus improving microcirculation. A good example of this is rosy cheeks when you come in from the cold. One major benefit of skin icing is the ability to reduce inflammation, meaning that many people who suffer from inflammatory skin conditions like acne and rosacea can benefit from cold therapy.
The only thing to note is that the effects don’t accumulate in the long term so it’s something you need to do for results, but you know, it can be your special treat for nights out or big events.








