Imperfect system and cruel barriers still stopping women access abortion
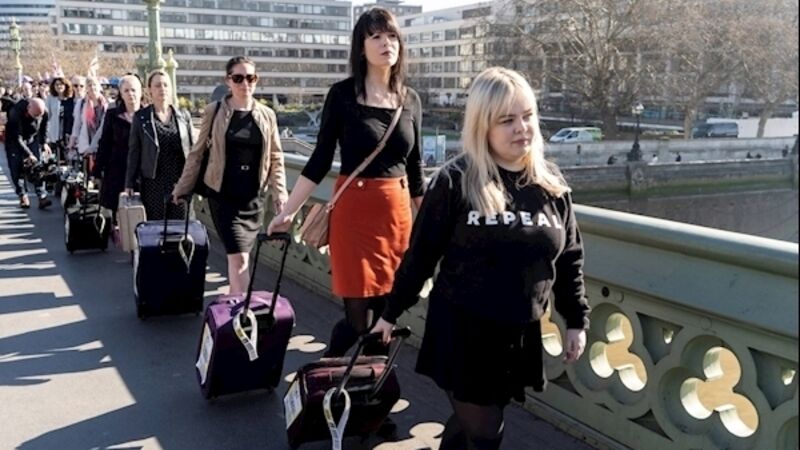
There has been a drop of up to 85% in the number of Irish women travelling to Britain for abortions, one year on since the Eighth Amendment was repealed from the Irish Constitution.
Nine women had been leaving Ireland every day to have a termination in Britain.










