Mental Health Commission of Ireland: Patients spending too long in mental health units
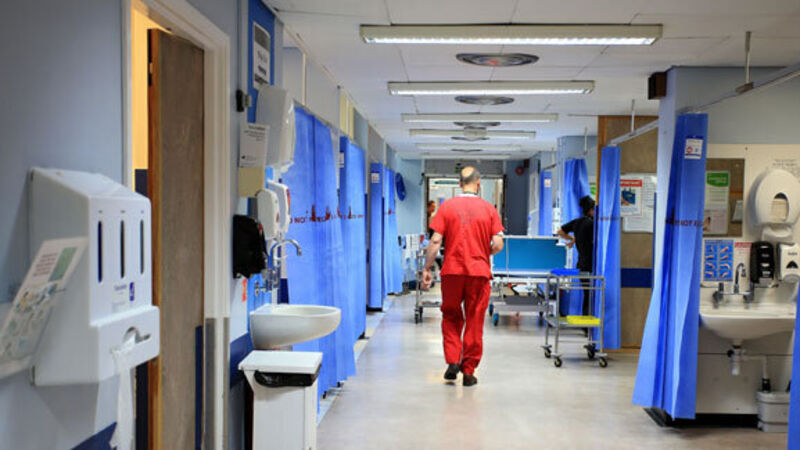
People are spending more time in acute mental health units than they need to, according to the Mental Health Commission of Ireland.
This is because there is an almost “total absence” of community mental health support services across the State, it stated.
Access to acute beds is being restricted as a result — leading to overcrowding in acute adult mental health services. It has also led to more people with mental health problems being treated in the general hospital population.
Regulator John Farrelly said this is an inappropriate setting in which to treat mental health patients, pointing out that the agreed public policy that should be in place to cover his concerns has “simply not been implemented”.
The policy document, A Vision For Change, was published in 2006, but little or nothing ever came of it.
Very few of the support services — including so-called ‘crisis houses’, intensive high-support hostels, specialist rehabilitation units, and psychiatric intensive care units — even exist.
“The HSE is responsible for implementing public policy, but it simply hasn’t done its job and I don’t think anybody is being held to account,” said Mr Farrelly.
“The Vision For Change policy was signed off and agreed in 2006. I am aware there is yet more mental health policy coming down the tracks, but why on Earth don’t we implement the policy that we already have?
“The only way this is going to work is if more buildings are built and for there to be a serious recruitment drive.
Unfortunately, while politicians love talking about mental health, it is absolutely the Cinderella service of the health service. It is just so wrong on so many fronts that people are being left in acute mental health units who simply do not need to be there.
When it was published, A Vision For Change promised that “every citizen should have access to local, specialised, and comprehensive mental health service provision that is of the highest standard”.
Its publication came nearly three years after the 2003 Expert Group on Mental Health Policy was set up to “formulate a blueprint for a world-class service to meet the mental health challenges facing our society”.
Two years ago, the chairwoman of that expert group, Joyce O’Connor, said there were issues with implementing the policy.
“The big problem has been in implementation,” she told members of the Joint Committee on Future of Mental Health Care in 2017.
The Mental Health Commission report warns: “Where a lack of specialised supports exist, many immediate and long-term consequences ensue for acute mental health beds.”
Last night, the HSE said in a statement: “We provide a wide range of community mental supports across the state. Nationally, there is a total of 111 general adult community teams, 32 psychiatry of later life teams and 71 child and adolescent community teams. These teams support people to remain in their homes and in the community where possible in line with Sláintecare.”
The HSE added that it seeks to “enhance our comprehensive range of community mental health supports and specialist services” on an ongoing basis.














